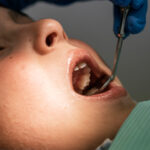
You did it. You faced the dreaded tooth extraction, and now you’re recovering. While some discomfort is normal, a sharp, throbbing, and persistent pain that starts a few days later can be terrifying. You may be wondering: Is this just normal tooth extraction pain, or is it a dry socket?
For patients in Madison, New Jersey, and the surrounding areas of Chatham, Morristown, Florham Park, and Summit, understanding the critical signs of this complication is essential for prompt treatment and relief.
At Madison Dentistry & Implant Center, we know that when it comes to your oral health, clarity and fast action are key. This comprehensive guide, informed by our experts, will walk you through everything you need to know about dry socket symptoms, causes, prevention, and the effective, pain-relieving treatments we offer right here on Main Street. Don’t suffer in silence—let’s demystify this common post-operative complication and get you on the path to comfortable healing.
What Exactly is a Dry Socket (Alveolar Osteitis)?
The medical term for dry socket is Alveolar Osteitis. It is the most common complication following a permanent tooth extraction, particularly the removal of lower wisdom teeth.
The Essential Blood Clot
Normally, after a tooth is removed, a blood clot immediately forms in the empty socket (the hole in the bone). This dark, jelly-like clot is a protective scab—it covers and shields the underlying bone, nerves, and soft tissue. It also acts as the foundation for new tissue to grow, which is critical for the healing process.
The Complication: Dislodged or Dissolved Clot
A dry socket occurs when this essential blood clot either fails to form initially or, more commonly, becomes dislodged or dissolves before healing is complete. This leaves the sensitive underlying bone and nerve endings exposed to air, food particles, and liquids, leading to intense, radiating pain that over-the-counter pain medications simply can’t touch.
While general post-extraction pain peaks within the first 24-48 hours and then subsides, dry socket pain typically begins or dramatically worsens 1 to 3 days after the procedure. This timing is your first major clue.
The Telltale Dry Socket Symptoms: How to Spot the Danger Signs
Identifying the problem early is the best way to get fast relief. If you’ve recently had a tooth pulled at a dental office in Madison, New Jersey, or any nearby town, monitor closely for the following definitive dry socket symptoms.
1. Severe, Throbbing, and Worsening Pain
The single most defining characteristic of dry socket is the intensity and nature of the pain.
- Timing: Pain starts or worsens significantly on day 2 or 3 post-extraction.
- Quality: It is typically described as a severe, deep, throbbing ache that escalates instead of improving.
- Lack of Relief: The pain is usually not manageable with the over-the-counter pain relievers (like ibuprofen or acetaminophen) that controlled your initial post-operative discomfort. Many patients find it so severe it disrupts sleep and daily function.
2. Pain Radiating to Other Areas
The exposed nerves transmit pain beyond the immediate extraction site. You may feel the sharp ache spreading from the socket to other parts of your face and head:
- The Ear
- The Temple
- The Eye (on the same side of the face)
- The Neck or Jaw
3. A Visibly Empty Socket (The “Dry” Look)
This is the literal sign of the condition:
- Absence of the Clot: You may look into the extraction site and see a hole that appears empty. Instead of the dark red or dark brown clot, you might see a pale, white, or grayish layer.
- Visible Bone: In clear cases, you may be able to see the exposed bone at the bottom or sides of the socket.
4. Foul Odor and Unpleasant Taste
As the exposed socket struggles to heal and food debris may collect in the empty space, bacteria can thrive. This results in:
- Halitosis (Bad Breath): A noticeable, foul odor coming from the mouth that is worse than typical morning breath.
- Dysgeusia (Bad Taste): A persistent, unpleasant, metallic, or stale taste in your mouth that is difficult to wash away.
If you recognize any combination of these dry socket symptoms, particularly the severe, radiating pain that kicks in after the first two days, do not delay—contact a dental professional immediately.
The Causes and Risk Factors: Why Does the Clot Dislodge?
Understanding the common culprits behind a dry socket is the first step toward prevention. While the exact biological mechanism isn’t fully understood, certain actions and patient factors significantly increase the risk.
Behavioral and Mechanical Factors
These are the most common, and most preventable, causes:
- Sucking Actions: The negative pressure created by drinking through a straw, rinsing vigorously, or forceful spitting can easily dislodge the delicate blood clot. This is the single biggest mechanical risk.
- Smoking and Tobacco Use: The chemicals in tobacco constrict blood vessels, inhibiting the blood clot from forming and slowing down the overall healing process. Furthermore, the sucking action required to inhale from a cigarette is a powerful mechanical dislodger. This is considered the number one risk factor.
- Poor Oral Hygiene: Pre-existing infection or poor hygiene after the procedure can introduce bacteria that break down the clot prematurely.
Patient-Specific and Surgical Risk Factors
- Location of Extraction: Dry socket is far more common after the removal of lower wisdom teeth (mandibular third molars) due to the dense bone structure and reduced blood supply in the area.
- Difficult Extraction: A traumatic or lengthy extraction, often required for impacted teeth, can lead to increased inflammation and risk.
- Prior History: If you’ve had a dry socket before, your chances of developing it again are significantly higher.
- Hormonal Factors: Women who use oral contraceptives (birth control pills) are at an increased risk due to elevated estrogen levels, which can interfere with the clotting process.
Prevention is the Best Medicine: Post-Extraction Care Guidelines
Preventing a dry socket starts the moment you leave the dental chair. Following your post-operative instructions from your Madison Dentistry & Implant Center dentist is crucial.
Golden Rules for the First 48 Hours
- NO Smoking or Tobacco: Absolutely refrain from all tobacco products for at least the first 48 hours—ideally for a week.
- NO Straws: Avoid drinking from a straw or creating any sucking motion. Sip liquids gently.
- NO Forceful Rinsing or Spitting: If you need to rinse, simply tilt your head gently and let the liquid run out. Do not swish violently.
- Manage Bleeding: Bite down firmly but gently on the gauze provided for the first few hours.
- Diet: Stick to soft, cool foods like yogurt, mashed potatoes, applesauce, and soup (not hot) for the first 24-48 hours. Avoid crunchy, hard, or chewy foods that could irritate the site or leave particles behind.
- Rest: Limit physical activity and strenuous exercise for several days.
Ongoing Hygiene and Care
- Gentle Cleaning: Brush your teeth carefully, avoiding the extraction site. Start gentle warm salt water rinses (1/2 teaspoon of salt in a glass of warm water) 24 hours after surgery, several times a day, to keep the area clean.
- Medication: Take all prescribed antibiotics and pain relievers exactly as directed by your Madison, NJ dentist.
Expert Dry Socket Treatment in Madison, NJ: Finding Relief
If you suspect you have a dry socket, the most important step is to call Madison Dentistry & Implant Center right away. Do not attempt to treat it yourself with objects or aggressive rinsing. Prompt, professional treatment provides immediate and lasting relief.
The Dentist’s Approach to Pain Relief
Treatment is focused on two goals: immediate pain relief and promoting healing.
- Cleaning and Irrigation: The dentist will gently flush (irrigate) the socket to remove any trapped food debris or bacteria. This is often done using a special medicated rinse or saline solution.
- Medicated Dressing (Packing): This is the key to relief. The socket is gently packed with a medicated paste, gel, or dressing. This specialized material usually contains an antiseptic to protect the exposed bone and a powerful numbing agent (like eugenol or lidocaine) to provide almost instantaneous relief from the intense pain.
- Dressing Changes: You may need to return to the clinic for dressing changes every 24 hours until the severe pain is gone.
- Home Care Instructions: Your dentist may give you a curved-tip syringe for gently flushing the socket at home with warm salt water after the initial packing is removed.
While dry socket is painful, it is highly treatable. Once the bone is protected with the medicated dressing, pain typically subsides significantly within a few hours, and complete healing usually occurs within 7 to 10 days of starting treatment.
Your Local Emergency Dental Resource in New Jersey
If you are experiencing severe tooth extraction pain in Madison, or in nearby communities like Chatham, Morristown, Florham Park, or Summit, you need a responsive, professional team. At Madison Dentistry & Implant Center on Main Street, we specialize in comprehensive general and specialty care, including wisdom tooth extractions and treating complications like alveolar osteitis.
Our state-of-the-art facility is equipped to diagnose and treat your dental emergency quickly, getting you the relief you need when you need it most. When you search for ‘Dry Socket Treatment near me’, know that our team is prepared to offer exceptional care for all patients in the Morris County area.
Frequently Asked Questions (FAQs) About Dry Socket
How long does a dry socket last?
Once treatment—specifically the medicated dressing—begins, the severe pain should subside rapidly. The socket itself typically heals within 7 to 10 days from the start of treatment, as new tissue grows to cover the exposed bone.
Does a dry socket heal on its own without a dentist?
A dry socket can eventually heal on its own, but this process is much slower and incredibly painful. The primary goal of visiting the dentist is to get the medicated packing which provides immediate pain relief and protects the exposed area to speed up healing. It is strongly advised to seek professional treatment.
When should I worry about pain after my tooth extraction?
A certain amount of pain is normal for the first 1-2 days. You should worry, and contact your dentist, if:
- The pain is severe, throbbing, and debilitating.
- The pain worsens dramatically on day 2 or day 3, instead of improving.
- The pain radiates to your ear, temple, or neck.
- You can see a visibly empty socket or exposed bone.
Can I get a dry socket from a routine filling or crown?
No. Dry socket is a complication that can only occur after a tooth extraction where the root of the tooth has been pulled, leaving an open socket in the jawbone. It cannot happen after a simple filling, crown, or deep cleaning.
Conclusion: Prioritize Your Comfort and Healing
A tooth extraction is a significant step toward a healthier smile, but complications like dry socket can be a painful setback. By understanding the key dry socket symptoms—the worsening, radiating pain, the foul odor, and the empty socket—you are empowered to seek prompt help.
Do not tough it out. If you suspect you have Alveolar Osteitis following a procedure, the expert team at Madison Dentistry & Implant Center is here to provide the compassionate and effective dry socket treatment you need. Serving our community in Madison, New Jersey, and patients from Chatham, Florham Park, Morristown, and Summit, our priority is getting you out of pain and back to your life. Contact us today!