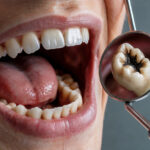
Dental implants are widely considered the gold standard in modern restorative dentistry. They offer a permanent, natural-looking, and fully functional solution for missing teeth. With a success rate hovering around 95% to 98%, it is easy to see why millions of people choose implants to restore their smiles. However, just like natural teeth, dental implants require meticulous care and attention. When they are neglected or when certain risk factors are present, a complication known as a dental implant infection can occur.
If you are experiencing discomfort around your implant, or if you simply want to educate yourself on how to protect your investment, you are in the right place. At Madison Dentistry & Implant Center in Madison, New Jersey, we believe that patient education is the first line of defense. In this comprehensive guide, we will explore everything you need to know about dental implant infections—from the early warning signs to the latest treatment protocols—so you can keep your smile healthy and radiant for a lifetime.
What is a Dental Implant Infection?
A dental implant infection is an inflammatory condition that affects the soft and hard tissues surrounding a dental implant. In the dental world, this condition is broadly categorized into two distinct stages:
1. Peri-Implant Mucositis
This is the early stage of a dental implant infection. It is remarkably similar to gingivitis in natural teeth. During this phase, the bacterial plaque builds up around the base of the implant, causing inflammation in the soft gum tissue. The good news? Peri-implant mucositis is entirely reversible if caught early and treated with proper professional care and an improved home oral hygiene routine. At this stage, the underlying jawbone remains unaffected.
2. Peri-Implantitis
If peri-implant mucositis is left untreated, it can evolve into peri-implantitis. This is a much more severe condition. At this stage, the infection has progressed beyond the gums and has begun to attack and degrade the jawbone supporting the titanium implant post. Because the implant relies on this bone for stability (a process called osseointegration), bone loss can ultimately lead to the failure and necessary removal of the implant. Peri-implantitis requires immediate, aggressive intervention by an experienced dental professional.
Top Signs and Symptoms You Shouldn’t Ignore
Catching an infection early is the key to saving your dental implant. Because implants do not have nerves like natural teeth, you won’t feel a “toothache” in the traditional sense. Instead, you must rely on observing the surrounding tissues. Watch out for these telltale signs of a dental implant infection:
- Red, Swollen, or Tender Gums: Healthy gums should be firm and pale pink. If the gums around your implant look intensely red, puffy, or feel tender to the touch, inflammation is present.
- Bleeding When Brushing or Flossing: Just like with natural teeth, bleeding gums are one of the earliest signs of gum disease and implant infection.
- Pus or Discharge: If you notice pus oozing from the gums around the implant, or if you frequently experience a foul taste in your mouth, this is a clear indicator of a bacterial infection.
- Persistent Bad Breath: Medically known as halitosis, bad breath that doesn’t go away with brushing or mouthwash can be caused by the bacteria thriving in the infected periodontal pockets.
- Throbbing Pain or Discomfort: While the implant itself lacks nerves, the surrounding gums and bone do not. A throbbing sensation or pain when chewing is a red flag.
- A Loose or Shifting Implant: This is a late-stage symptom indicating significant bone loss (peri-implantitis). If your implant feels wobbly, you need to contact your dentist immediately.
- Visible Threads: If the gums recede enough that you can see the gray, threaded titanium body of the implant, the supporting structures are failing.
Causes and Risk Factors: Why Do Implants Get Infected?
Understanding the root cause of a dental implant infection is vital for both treatment and prevention. The primary culprit is always bacteria, specifically the biofilm (plaque) that accumulates at the gum line. However, several risk factors can dramatically increase your chances of developing an infection:
Poor Oral Hygiene
This is the number one cause of implant failure. If you do not brush and floss around your implants daily, plaque will harden into tartar, creating an ideal breeding ground for destructive bacteria.
Smoking and Tobacco Use
Smoking is notoriously detrimental to oral health. It restricts blood flow to the gums, depriving them of the oxygen and nutrients needed to fight off infections and heal properly. Smokers are at a significantly higher risk of developing peri-implantitis compared to non-smokers.
A History of Periodontal (Gum) Disease
If you lost your natural teeth due to severe gum disease, you are naturally more susceptible to developing an infection around your implants. The bacteria that caused your initial tooth loss can still reside in your mouth and attack your new implants.
Uncontrolled Diabetes
Diabetes affects the body’s ability to heal and fight off infections. Patients with uncontrolled blood sugar levels face a much higher risk of implant complications.
Bruxism (Teeth Grinding)
Chronic teeth grinding or clenching puts immense, unnatural pressure on the dental implant. Over time, this micro-movement can loosen the implant and create tiny spaces between the implant and the bone where bacteria can infiltrate.
Actionable Tips to Prevent Dental Implant Infections
At Madison Dentistry & Implant Center, we emphasize that proactive prevention is always better, easier, and more cost-effective than reactive treatment. Here are our expert, actionable tips to keep your implants infection-free:
- Upgrade Your Brushing Technique: Brush at least twice a day using a soft-bristled toothbrush. Consider switching to an electric toothbrush, which is generally more effective at removing plaque than manual brushing. Use a low-abrasive toothpaste to avoid scratching the crown.
- Embrace Interdental Cleaning: Standard dental floss is great, but water flossers (like a Waterpik) are absolute game-changers for implant patients. They use a targeted stream of water to flush out bacteria and food particles from deep pockets that traditional floss might miss.
- Use Interproximal Brushes: These tiny, cone-shaped brushes are perfect for cleaning the hard-to-reach spaces between your implant and your natural teeth. Ensure the wire is nylon-coated so it doesn’t scratch the titanium implant post.
- Quit Smoking: If you smoke, quitting is the single best thing you can do to protect your implants and your overall health. Ask your doctor for cessation resources.
- Wear a Nightguard: If you grind your teeth at night, a custom-fitted nightguard will protect your implants from excessive bite forces and micro-trauma.
- Maintain Regular Dental Checkups: Do not skip your bi-annual cleanings! Professional dental hygienists use specialized tools (often made of plastic or resin so they don’t scratch the implant) to safely remove hardened tartar that you simply cannot remove at home.
Treatment Options at Madison Dentistry & Implant Center
If you suspect you have a dental implant infection, time is of the essence. Depending on the severity of the infection, treatment options vary. Our team at Madison Dentistry & Implant Center utilizes state-of-the-art technology to provide the most effective care possible.
- Professional Debridement: For early-stage mucositis, we will perform a deep, thorough cleaning of the implant surface to remove plaque, tartar, and bacterial biofilm.
- Antibiotic Therapy: We may prescribe local or systemic antibiotics to help eradicate the stubborn bacteria causing the infection. Antimicrobial mouth rinses are also highly effective.
- Surgical Intervention: In advanced cases of peri-implantitis where bone loss has occurred, surgical intervention may be required. This can involve opening the gums to thoroughly clean the implant surface, followed by bone grafting to regenerate the lost bone structure.
- Implant Removal: In the absolute worst-case scenario where the bone loss is too severe and the implant has completely failed, it may need to be carefully removed. After a period of healing and potential bone grafting, a new implant can often be placed.
Your Trusted Implant Experts in New Jersey
When dealing with something as complex as a dental implant infection, you need a team you can trust. Madison Dentistry & Implant Center, proudly located in the heart of Madison, New Jersey, is dedicated to providing top-tier, compassionate periodontal and implant care.
We don’t just serve Madison; we are the go-to implant specialists for residents in the surrounding communities, including Chatham, Florham Park, Morristown, Summit, and Short Hills. Whether you need your very first implant consultation, routine maintenance, or specialized treatment for an infected dental implant, our local clinic offers the advanced technology and personalized care required to protect your smile. Because we are conveniently located, our patients from Morristown and Chatham never have to travel far to receive world-class dental interventions.
TL;DR: Key Takeaways
Short on time? Here is what you need to remember about dental implant infections:
- Two Stages: Infections start as reversible peri-implant mucositis (gum inflammation) and can progress to severe peri-implantitis (bone loss).
- Watch the Signs: Bleeding gums, redness, swelling, bad breath, and pus are major warning signs. Never ignore a loose implant.
- Hygiene is Everything: Poor oral hygiene and smoking are the biggest risk factors.
- Prevention is Easy: Use a soft-bristled brush, a water flosser, and keep up with your professional cleanings every six months.
- Act Fast: If you suspect an infection, contact Madison Dentistry & Implant Center immediately. Early intervention saves implants.
Frequently Asked Questions (FAQs)
Can a dental implant infection clear up on its own?
No. While minor gum irritation might subside, a true bacterial infection around an implant requires professional intervention. Ignoring it will only lead to bone loss and eventual implant failure.
Is it painful to treat an infected dental implant?
Patient comfort is our top priority. Treatments are performed under local anesthesia, ensuring you feel little to no discomfort during the procedure. Post-treatment soreness is usually mild and easily managed with over-the-counter pain relievers.
How long does it take for an implant to get infected?
It varies. An infection can develop just a few weeks after surgery if post-operative care instructions aren’t followed, or it can happen years later due to a lapse in oral hygiene or changes in health (like developing diabetes).
Can an implant be saved if it gets infected?
Yes, absolutely—if caught early! If the infection is limited to the gums (mucositis), it is highly treatable. Even early-stage peri-implantitis can be halted with laser therapy and deep cleaning. However, if bone loss is severe, the implant may need to be removed.
Conclusion
Dental implants are a spectacular investment in your health, confidence, and quality of life. However, they are not entirely maintenance-free. Understanding the signs of a dental implant infection and knowing how to prevent one through diligent home care and regular professional checkups is the secret to making your implants last a lifetime.
If you are experiencing any redness, bleeding, or discomfort around your dental implant, do not wait for the situation to worsen. Procrastination is the enemy of a healthy smile.
Are you ready to protect your smile? Contact Madison Dentistry & Implant Center in Madison, NJ, today to schedule a comprehensive evaluation. Whether you are coming from Chatham, Morristown, Summit, or right here in Madison, our expert team is ready to restore your oral health.